By Kate Robards, AASM Senior Writer
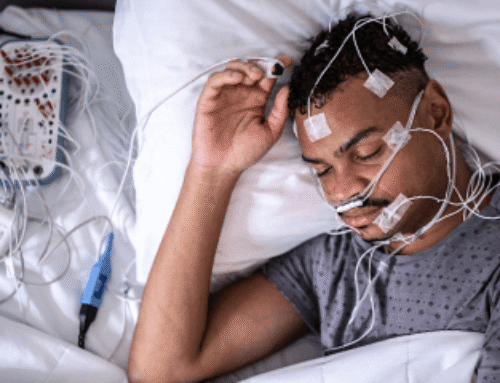
According to AASM membership data, about 25% of AASM members are in private practice. As advancements in sleep technology allow for more flexibility, more members are considering this practice model. Despite alluring benefits like more autonomy and better patient engagement, private practice professionals also face insurance frustrations and rising cost concerns.
Choosing independence
Some practitioners believe that, without the bureaucratic red tape in place at larger institutions, being in private practice allows for the ability to provide better care to patients and adapt to change faster.
For Matthew Troester, DO, FAASM, the allure of private practice was about getting back to basics.
After nearly two decades in academic neurology, Dr. Troester shifted to private practice, co-founding a business in Scottsdale, Arizona, with his wife Ashesh Troester, PA-C, who’s also a sleep medicine professional and AASM member.
“Our mission statement is to provide excellent care and promote healthy sleep by nurturing a partnership with our patients, one at a time. We are not focused on growth. We are not focused on being acquired. We simply want to take care of people efficiently and effectively,” Dr. Troester said. “This strategy alone has provided the biggest benefit, which was honestly somewhat unexpected, although we had hoped it might work out that way.”
The improvement to patient care is one of the aspects that attracted Christopher Winter, MD, FAASM, to private practice as well. In private practice since 2004, Dr. Winter is the owner of Charlottesville Neurology and Sleep Medicine clinic and CNSM Consulting.
Dr. Winter is not shy about enumerating the benefits of being in private practice; he has a list of his top 10 reasons, which include more control over the total medical experience of his patients.
Sahil Chopra, MD, CEO and co-founder of Empower Sleep, also believes that the private practice model is better for patient outcomes. He shared his experience on a recent episode of the AASM’s Talking Sleep podcast about embracing alternative practice models.
“When we have frequent touch points and we get to close the loop to see if something is working or not working, patient engagement seems to be much higher, outcomes seem to be much better,” Dr. Chopra said.
Joining Dr. Chopra on the episode was Andy Berkowski, MD, who also pointed to the ability to have more time and communication with the patient as a positive of his practice’s model.
In private practice, there’s more autonomy in decision making. There’s also the flexibility to not only set your own hours, but also shape your company’s culture. To Dr. Troester, this autonomy and resultant flexibility is one of the most obvious benefits of being in private practice.
“If we do not like how something is working, we change it. If we receive feedback that something we are doing could be better, we change that. If we want to take a vacation, we do. If we want to stop seeing patients at 2 p.m. on Wednesday for no reason, we can. We have the ability to be very dynamic with our decision-making,” he said.
Compensation is a top consideration when thinking about a move to private practice—but is it a pro or con? Pay may be similar for those in private practice compared to institutional or academic employment. In hospital and academic institutions, the administration will determine salary; in private practice, pay may fluctuate depending on patient load, revenue and overhead expenses.
Yes, you have to be prepared to let go of a regular paycheck and start at zero when making a move. While giving up a guaranteed salary may be uncomfortable, pay transparency may be gained.
Pay played a role in Dr. Troester’s shift into private practice. After an enjoyable two-decade career in academic medicine, his trigger was a long-looming cut in compensation.
“I figured if I was going to make less anyway, I might as well try to do it on my own and see what happens,” he said.
While income may not differ greatly, private practice professionals enjoy more autonomy, flexibility and improvements in patient relationships.
The challenges of running a private practice
There are, of course, many challenges to contend with as well.
At the forefront, there’s the cost. Opening a private practice requires a capital investment, and amid rising costs, there’s an elevated need to keep overhead expenses down. Pay may also fluctuate and depend on how many patients are seen and how many staff are in the office.
The administrative duties can be time-consuming as well. This may include everything from business operations, such as setting up a patient management system, to marketing. Managing a schedule, payroll, and billing can be a burden.
For Dr. Troester, the biggest frustration is getting patients to pay their copays, coinsurance and deductibles.
“On a day-to-day basis, this is surprisingly one of the more challenging aspects,” Dr. Troester said. “Patients pay large monthly premiums and do not always understand why they have to incur additional costs at time of service. We both find ourselves explaining the insurance system to really smart and savvy (and sometimes angry) patients lacking insight as to how their plan operates.”
Insurance poses a challenge for Dr. Winter as well. Earlier this year, he announced that his clinic is no longer accepting commercial medical insurance.
“As a small clinic, having to play by the ever-changing insurance rules and the inability to adjust what we charge for our labor-intensive services became too difficult,” Dr. Winter said. “There really was no choice. It was either change or go out of business. The model of insurance payments and delayed collections made billing difficult and unpredictable. We wanted a much simpler process.”
Prior authorizations, insurance denials, Medicare rules, and coding and billing requirements can pull time away from patient care. Faced with barriers created by insurance companies, others are turning to alternatives as well.
On Talking Sleep, Dr. Berkowski elaborated on the membership-based model that his direct specialty care clinic uses. More flexible than an insurance-based system, this model doesn’t bill insurance companies at all.
“It’s based on patient fees direct to the physician, and therefore it cuts down on a lot of the restrictions and requirements, and it frees us up to provide more timely care, more accessible care,” Dr. Berkowski said.
Other challenges may be related to treating specific sleep disorders, such as access to CBT-I specialists for patients with insomnia or the availability of iron infusion centers for those with restless legs syndrome.
While embracing alternative practice models may alleviate some of the challenges associated with private practice, the prospects of added responsibility and less financial security and support may be barriers for some.
Opportunities for growth
Combating these challenges is no small feat.
Dr. Troester has been able to automate many tasks, which has allowed his business to run lean.
“We anticipate additional automation as we get more comfortable with letting go of some control. We are trying to be automated in all the right ways and old-fashioned in all the others,” he said.
For those who are concerned about the overhead costs of starting a brick-and-mortar clinic, telemedicine provides an opportunity as well. Drs. Chopra and Berkowski both operate with telemedicine, which reduces costs.
While licensure restrictions that lifted temporarily during the COVID-19 pandemic are now back in place, there remains the opportunity to be licensed in multiple states to provide broader care via telemedicine. Dr. Chopra is licensed in 45 states!
The availability of wearable sleep technologies may also present an opportunity. These innovations may break down barriers to access while also improving patient outcomes. Dr. Chopra’s hyper-personalized model of care includes using novel sleep testing devices, such as Sleep Image and Cerebra.
“Similar to what continuous glucose monitors have done for diabetics, we’re trying to take that same approach to continuous sleep care,” Dr. Chopra said.
Similarly, the availability of home sleep apnea testing is opening doors for sleep medicine professionals who are forgoing polysomnograms and other expensive sleep study equipment. Home testing and remote monitoring present an opportunity to assess and treat patients more quickly while keeping expenses low.
Advice for successfully shifting to private practice
The advice from those who have made the jump into private practice resoundingly centers around believing in yourself and taking the leap.
“Just do it. Go for it. Walk into a motivational poster store, read 5 or 6 of them, go home, write your resignation letter, and take back all the control you have surrendered. You finished college, you finished medical school, you finished internship, residency and fellowship. You can totally do this; it is difficult, but doable. Do not be afraid,” Dr. Troester said.
Dr. Winter’s advice echoes this theme of facing your fears.
“Believe in yourself. I talk to many academic doctors who remain in bad jobs because they are scared. I do not think the average academic training program adequately educates and prepares doctors for the choice to go private. My program actively dissuaded me from doing it. I’m thankful every day I did, although I miss the free Grand Rounds pizza,” he said.
Dr. Chopra noted that building your motivation to try something new may be more difficult than managing the business side of a private practice. He, too, encourages those interested in exploring alternative models to go for it.
“If you don’t like what you do, something is wrong,” he said. “If you can get through med school and residency, you can persevere and try it.”
Talking to others in private practice can be invaluable as well. Visit the Members Forum discussion group in the AASM Engage platform to chat with members who have similar experiences and can provide insight and information.
This article appeared in volume eight, issue three of Montage magazine.