Fariha Abbasi-Feinberg, MD, FAASM, member of AASM Board of Directors
Over the course of my 25-year career in sleep medicine, I have navigated through several pivotal transitions, with each chapter presenting valuable insights.
I have experience as an owner/partner of a general neurology practice and an employed physician in an ENT practice, and I now practice within a group of health care providers, mainly consisting of colleagues in primary care. My present practice, Millennium Physician Group, is part of an Accountable Care Organization (ACO), a term I had previously heard but never fully comprehended. You may think this model does not concern you, but many of you work within systems that are part of an ACO. Fifty-eight percent of all community hospitals nationwide, and even a higher percentage of university centers, are part of an ACO. Your day-to-day activity and compensation may not yet be tied to ACO outcomes, but at some point this may change, and being proactive and informed is important.
What exactly is an ACO?
Health care payments have gone through a major shift over the last decade. Between the passage of the Affordable Care Act (ACA) and the Medicare Access and CHIP Reauthorization Act (MACRA), there has been a shift in payment from volume-based, fee-for-service to value-based payment. Alternate payment models include programs such as bundled payment options as well as ACOs. Simply put, an ACO is a group of providers that coordinates care for a specific group of patients. The goal is to improve health outcomes while keeping costs in check. ACOs focus on preventative care and reduction of costly hospitalizations.
How do ACOs achieve their goal?
ACOs use complex data analytics to monitor patient health, track care delivery, and identify areas for improvement. For instance, at Millennium Physician Group, we focus on making it easy for patients to get care, whether through same-day appointments, walk-in clinics, or a dedicated care team. This team includes not only the physicians and advanced practice providers but also home health care nurses, social workers, pharmacists, and coaches. Together they assist in choosing cost-effective medications, providing help with adherence, and assisting patients with all their health care needs.
Providers in the ACO are encouraged to meet quality and cost targets, which can lead to financial rewards. In an ACO model, providers receive fee-for-service payments throughout the year. If the ACO spends less than expected, the ACO earns the “shared savings” revenue. These payments are usually made annually.
A key component of an ACO is taking financial risks. This means they are not just focused on providing high-quality care but also on managing the cost of caring for their patients. The cost of care comes directly from the ACO. This includes services such as sleep studies and treatment for all sleep disorders.
ACOs can have different types of financial agreements. Some reward providers if they save money (upside) while others may require repayment if costs go over a certain limit (downside). The downside arrangements encourage ACOs to take on more responsibilities for cost management in exchange for a greater share of the savings.
How does sleep medicine fit into this model?
The manner in which specialists deliver services profoundly influences the ACO’s capacity to enhance quality and manage costs. Specialty care is significantly more expensive than primary care. In most ACOs, the majority of specialty care is provided outside of the ACO network. ACOs have therefore become increasingly interested in connecting with specialty physicians. ACOs that employ specialists are looking at new types of arrangements. For instance, some ACOs require that referrals be first discussed between the primary care provider and their employed specialists in a “curbside consult” to see if the PCPs can manage more care themselves. This is wonderful for patients because they can avoid both long wait times to see specialists and additional copayments. In some ACOs, specialists educate their primary care colleagues in a more formal fashion, providing the tools to help them manage patients.
The Centers for Medicare and Medicaid Services (CMS) and the American Medical Association (AMA) have also presented possible opportunities. The AMA has designed a program called Payments for Accountable Specialty Care (PASC), which allows primary care and specialty physicians to work together. The specialist would take responsibility for delivering services to improve outcomes and/or reduce avoidable spending. This is designed to improve services for the patient, and the specialists would receive an Enhanced Condition Services (ECS) payment in addition to the standard Medicare fee-for-service payment.
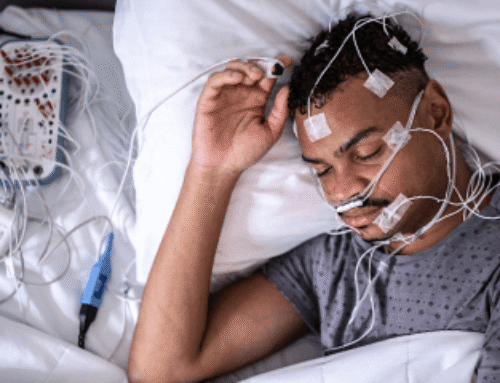
Sleep medicine could fit into this model effectively. Studies have shown that treating sleep disorders lowers health care costs. We have several options for providing cost-effective care. Our remote monitoring systems lend themselves perfectly to screen our population of patients and improve outcomes. We can help educate primary care providers to manage some sleep disorders effectively. With millions of undiagnosed patients with possible obstructive sleep apnea, we need to provide better access to care. We should work together with our primary care colleagues. Integration of sleep medicine into an ACO could be an interesting possibility.
The evolution of care models is a continuous process. ACOs may simply represent a chapter in the ever-evolving narrative of health care. To be prepared for the next chapter, we must actively engage in learning and participation.
Fariha Abbasi-Feinberg, MD, FAASM, is a sleep medicine specialist and a neurologist based in Florida. She is a member of the AASM Board of Directors.
This article appeared in volume eight, issue three of Montage magazine.