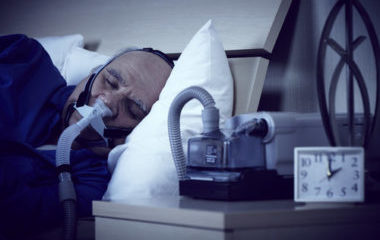
Consistent use of CPAP treatment in patients with known heart disease and newly diagnosed obstructive sleep apnea is associated with a lower likelihood of rehospitalization, according to a new study.
Results show that the risk of 30-day hospital readmission among those with cardiovascular disease and high adherence to CPAP for sleep apnea was 60% lower relative to those with low adherence to CPAP. The results highlight the importance of screening for and treating obstructive sleep apnea among individuals with cardiovascular disease, the authors wrote.
“Cardiovascular disease is the number one killer of older adults in the world,” said corresponding author Jennifer Albrecht, who has a doctorate in epidemiology and is an associate professor of epidemiology and public health at the University of Maryland School of Medicine in Baltimore. “Older adults with comorbid cardiovascular disease and obstructive sleep apnea are a vulnerable population at high risk for hospital readmission. Our data show that successful treatment of obstructive sleep apnea can greatly reduce the risk of 30-day hospital readmission.”
The study was published Aug. 8 as an accepted paper in the online Journal of Clinical Sleep Medicine. the official publication of the American Academy of Sleep Medicine.
Nearly 30 million adults in the U.S. have obstructive sleep apnea, a chronic disease that involves repeated collapse of the upper airway during sleep. It is found in 40%-60% of people diagnosed with cardiovascular disease. Obstructive sleep apnea is commonly treated with CPAP therapy, which uses mild levels of air pressure, provided through a mask, to keep the airway open during sleep.
The retrospective cohort study looked at Medicare recipients with cardiovascular disease who were newly diagnosed with obstructive sleep apnea between 2009 and 2013, initiated CPAP, and were hospitalized. Of the 1,301 patients who met the study criteria, the mean age was 73 years, and 53% were men. The 30-day readmission rate over the two-year period following CPAP initiation was 10.2%. Thirty-three percent of the study sample had low CPAP adherence, 38% had partial adherence, and 28.5% had high adherence. Relative to low adherence, Medicare beneficiaries with high adherence were 60% less likely to be readmitted to the hospital within 30 days.
“Obstructive sleep apnea is highly treatable, and treatment improves quality of life,” said Albrecht. “Treatment can also reduce 30-day readmissions, a major driver of health care costs in the U.S. If patients show signs of obstructive sleep apnea, such as snoring, daytime sleepiness, or poor sleep quality, they should talk to their doctor, and doctors should ask about sleep, especially when caring for older adult patients with cardiovascular disease.”
###
To request a copy of the paper, “Adherence to continuous positive airway pressure reduces the risk of 30-day hospital readmission among older adults with comorbid obstructive sleep apnea and cardiovascular disease,” or to arrange an interview with a study author or an AASM spokesperson, please contact the AASM at 630-737-9700 or media@aasm.org. Accepted papers, which are published online prior to their final inclusion in an issue, are not embargoed.
Established in 1975, the AASM advances sleep care and enhances sleep health to improve lives. The AASM has a combined membership of 11,000 accredited sleep centers and individuals, including physicians, scientists and other health care professionals who care for patients with sleep disorders. As the leader in the sleep field, the AASM sets standards and promotes excellence in sleep medicine health care, education and research.