By Kate Robards, Senior Writer
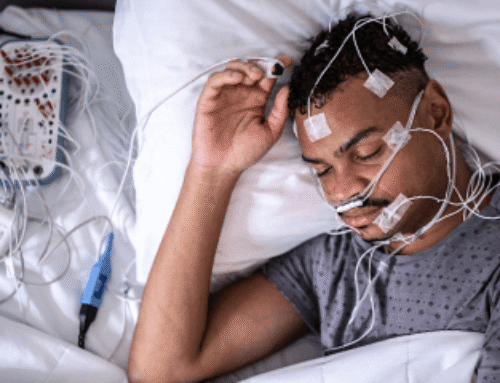
To determine the presence and severity of obstructive sleep apnea, health care professionals use a diagnostic tool known as the apnea-hypopnea index (AHI). AHI counts the number of apneas — periods when a patient stops breathing — and hypopneas — instances when the airway partially collapses, causing shallow breathing. Calculating AHI allows doctors to classify OSA severity.
While AHI is used in clinical practice, it’s been challenged in recent years for its inconsistent methodology. Variation in hypopnea measurement is a widely recognized concern.
An inability to account for all factors that underlie individual differences in response to OSA is another limitation of AHI. Emerging research suggests that, as a single metric, AHI cannot fully define the disease and its severity among a diverse patient population.
Despite these limitations, the AHI has been used for decades. However, with precision medicine on the rise, there’s an opportunity to develop a more nuanced, multidimensional approach to patient diagnosis and care.
The Sleep Research Society published a workshop report on metrics of sleep apnea severity in 2021.1 Currently, the Re-Envisioning OSA Characterization Task Force of the AASM is exploring the development of an updated framework for the characterization of OSA.
Several research groups are exploring novel or supplemental metrics to the AHI. Montage interviewed the lead authors of three recent studies to share highlights of potentially viable alternatives — or additions — to the AHI.
Ankit Parekh, PhD
Your research team at Mount Sinai developed an automated breath-by-breath measure called ventilatory burden, which may be a viable alternative to the AHI. Can you explain how the novel measure assesses the severity of OSA? Does it have the potential to replace AHI?
The automated measure that we have developed, termed ventilatory burden (VB), describes the proportion of small breaths overnight in an obstructive sleep apnea patient. Our data show that VB purely characterizes the reductions in airflow at the core of OSA. Our breath-based approach captures reductions in airflow independent of the presence of hypoxemia or arousal, without the need for subjective definitions of “baselines” that are utilized for event-based approaches, even if automated, and as such free of noise that potentially limits the utility of the AHI or other similar event-based measures.
In our paper,2 we have systematically investigated whether VB can be a viable alternative to the AHI. We have derived normal/abnormal cutoffs using VB as the disease definition for OSA, the relationship of VB to differing levels of upper airway obstruction via manipulation of the CPAP levels, its reliability night-to-night, and its prognostic utility. Our data suggest that indeed VB can be a viable and simple alternative to the AHI.
Winfried Randerath, MD
Your research team proposed a multicomponent grading system known as Baveno classification to characterize OSA. Can you describe the Baveno classification system? How does the Baveno system compare to AHI?
There is growing evidence on the limitations of the AHI. It is poorly associated with patient-related outcome measures, complications and outcomes. The Baveno classification (BC) has been proposed as an alternative guide to treatment indication.3 While the AHI determines the OSA diagnosis, the BC recommends treatment based on the severity of symptoms (e.g., sleepiness, insomnia, impaired driving ability) and cardiovascular/metabolic comorbidities (atrial fibrillation, heart failure, stroke, diabetes). Patients with minor symptoms and no or stable comorbidities are assigned to group A without treatment indication, those with severe symptoms and substantial or unstable comorbidities to group D with clear recommendation to treat – in both cases independent of the AHI. Treatment should be discussed individually in group B (severe symptoms, limited comorbidities) and C (minor symptoms, severe comorbidities). The evaluation of BC based on the European Sleep Apnoea Database (ESADA) shows a significant improvement of sleepiness in B and D and of blood pressure in C and D under treatment.4 This proves that treatment indicated based on relevant parameters rather than guided by the AHI alone results in substantial improvement of outcome. The BC also sufficiently demonstrates the heterogenous long-term course of untreated OSA patients.5 Future advancements of the BC include a more precise differentiation of the cardiovascular risk and the consideration of very high numbers of breathing disturbances.
Ali Azarbarzin, PhD
Your research team developed an OSA severity measure, the hypoxic burden, to characterize the underlying pathology of OSA. Can you tell us about your research and its implications for patient care? How does hypoxic burden compare to AHI in terms of predictive value for cardiovascular mortality?
OSA is characterized by repeated upper airway obstructions during sleep leading to frequent oxygen desaturations. Research from our group shows a strong association between the severity of airway obstruction (reduction in breathing) and degree of oxygen desaturation in population-based studies. Therefore, we designed the “hypoxic burden” of sleep apnea, defined as the total area under oxygen desaturation curve associated with all apneas and hypopneas (regardless of oxygen desaturation or arousal) to better capture the severity of OSA. In several population-based and clinic-based studies in the U.S. and Europe, our team and others have shown that hypoxic burden is strongly associated with incident cardiovascular disease and mortality, while AHI is not. The AHI considers all respiratory events equal, while there is substantial within and between-subjects variability in the severity of events and their acute and chronic impact on the cardiovascular system. Our recent post-hoc analysis of a randomized controlled trial of CPAP in patients with acute coronary syndrome and OSA shows that a high hypoxic burden predicted CPAP benefit (reduced risk of heart attack, stroke or heart failure).6 Despite these promising results, future randomized controlled trials in diverse samples are needed to prospectively confirm these findings.
Ankit Parekh, PhD, is assistant professor of medicine in the division of pulmonary, critical care and sleep medicine and assistant professor in the department of AI and human health at Icahn School of Medicine at Mount Sinai.
Winfried Randerath, MD, FERS, FCCP, FATS, FAASM, is professor and medical director at Bethanien Hospital in Germany and medical director at Institute of Pneumologie at the University of Cologne.
Ali Azarbarzin, PhD, is assistant professor of medicine at Harvard Medical School and lead investigator in the division of sleep and circadian disorders at Brigham and Women’s Hospital.
This article appeared in volume nine, issue one of Montage magazine.
References
- Malhotra A, Ayappa I, Ayas N, et al. Metrics of sleep apnea severity: beyond the apnea-hypopnea index. Sleep. 2021;44(7):zsab030. https://doi.org/10.1093%2Fsleep%2Fzsab030
- Parekh A, Kam K, Wickramaratne S, et al. Ventilatory Burden as a Measure of Obstructive Sleep Apnea Severity Is Predictive of Cardiovascular and All-Cause Mortality. Am J Respir Crit Care Med. 2023;208(11):1216-1226. https://doi.org/10.1164/rccm.202301-0109oc
- Randerath W, Bassetti CL, Bonsignore MR, et al. Challenges and perspectives in obstructive sleep apnoea: Report by an ad hocworking group of the Sleep Disordered Breathing Group of the European Respiratory Society and the European Sleep Research Society. Eur Respir J. 2018;52(3):1702616. https://doi.org/10.1183/13993003.02616-2017
- Randerath WJ, Herkenrath S, Treml M, et al. Evaluation of a multicomponent grading system for obstructive sleep apnoea: the Baveno classification. ERJ Open Res. 2021;7(1):00928-2020. https://doi.org/10.1183/23120541.00928-2020
- Serino M, Cardoso C, Carneiro RJ, et al. OSA patients not treated with PAP – Evolution over 5 years according to the Baveno classification and cardiovascular outcomes. Sleep Med. 2021;88:1-6. https://doi.org/10.1016/j.sleep.2021.09.010
- Pinilla L, Esmaeili N, Labarca G, et al. Hypoxic burden to guide CPAP treatment allocation in patients with obstructive sleep apnoea: a post hoc study of the ISAACC trial. Eur Respir J. 2023;62(6):2300828. https://doi.org/10.1183/13993003.00828-2023