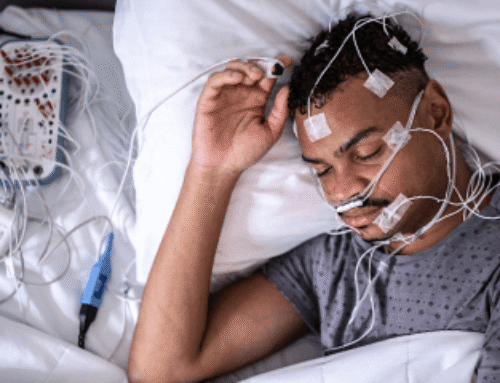
Brandon Peters, MD, FAASM, is a board-certified neurologist and sleep physician who practices at Virginia Mason Franciscan Health in Seattle. Dr. Peters helped steer the development of the sleep tracking algorithm used by Halo Rise, a bedside device released by Amazon in September 2022. The Montage team reached out to Dr. Peters to learn more.
How did you become involved with Amazon in the development of Halo Rise, and what role did you play?
I began my consulting role with Amazon in 2018. It is a collaboration that evolved over the years as my role in developing sleep-related devices and services expanded. Initially my work portfolio focused on the launch of the Halo Band, Amazon’s first wearable device designed to track and optimize various health metrics – including sleep. Beyond optimizing device accuracy, it was necessary to design and iterate the components of the sleep score algorithm and an associated recommendation engine. More recently, the contact-free sensor-based tracker and sunrise alarm called Halo Rise moved from the drawing board to reality with an expanding collection of capabilities and services to improve sleep. As these devices more fully integrated into Amazon’s suite of consumer-focused health offerings, the stewardship of this advancing technology was an exciting opportunity and responsibility.
What do you think was the most important contribution you made to the development of the device?
I am uniquely positioned as a clinician who has both a deep understanding of the foundational sleep science as well as the practical application of this knowledge. It was my daily task to ensure that the technology we developed at Amazon had grounding in the best available science. With our extensive resources and extraordinary expertise, we were often able to push this science forward. Beyond our internal validation studies, we launched important academic clinical research trials.
Did you learn anything from this experience that will benefit you as a clinician?
As a sleep physician, I may acknowledge the importance of the sleep environment in my discussion with patients, but I rarely have objective measurements of these variables. Clearly light has a profound effect on the circadian system and sleep quality, but who is able to report this over time? Similarly, bedroom temperature and humidity may be impactful unknowns. These insights may connect to the social determinants of health, including the built environment and other community concerns. This experience has led me to reflect on what constitutes optimal sleep quality and what levers lead to night-by-night and inter-individual variability.
How do you think sleep clinicians can more effectively use the data gathered by sleep trackers?
In a busy clinic day, the provider may shudder as the patient reaches out with sleep data collected by their devices, summarized by varying means, and displayed on their smartphone apps. At best, a cursory glance and vague platitudes may be offered. At worst, the information (and, by extension, the patient) may be summarily dismissed. What a lost opportunity! These devices allow longitudinal, real-world assessments of sleep with the integration of variables that impact sleep and health that have not been historically assessed. What does it mean when you have not one night of observation, but potentially hundreds? This may not only identify potential problems but allow longitudinal tracking of change and the successful targeting of interventions. The challenge of connecting real-world data and clinical acumen is an exciting one.
Do you think sleep trackers will have a more prominent clinical role in the future?
There is no doubt that sleep trackers of various stripes will continue to be integrated into the home environment and that the collected insights will lead many people to seek medical care. There is an expertise gap, too often filled by those without the education, experience, or insight to provide appropriate guidance. We must present the most comprehensive approach to provide the best care to our patients. Technology allows us to leverage the best available science and put this directly in the hands of our patients. I envision these trackers will continue to evolve to provide personalized, actionable guidance to users. When necessary, we will next be able to extend innovative services for the identification and management of sleep disorders and, more generally, inspire discussions between patients and their doctors around sleep quality and good health.
Do you have any advice for sleep clinicians who would like to be more involved in the development of new sleep devices?
Admittedly, I occupied an enviable position. For those who wish to pursue the advancement of sleep-related technology, reach out to leaders in the area of interest. In simple terms, put yourself out there. Attend relevant lectures at national meetings and pull the speakers aside afterwards. Consider creating an online presence with a personal site, social media involvement, interviews, and article contributions. If able, participate in the relevant AASM committees to learn more about these developing areas. Above all else, keep yourself grounded in science and in all things preserve a reputation for excellence.
This article appeared in volume eight, issue one of Montage magazine.