By the Coding and Reimbursement Advisory Committee
Billing pitfalls
As with many evolving telehealth services, billing for e-visits can be challenging. Practices frequently encounter denials or compliance concerns if they fail to follow the detailed rules. The most common pitfalls fall into four categories: inaccurate patient information, incomplete coding, consent issues, and administrative errors.
- Inaccurate patient and insurance data: One of the most frequent errors occurs when front-end staff enter incomplete or outdated demographic or insurance information. Failing to verify that the patient is still covered under a particular health plan or entering subscriber details incorrectly can cause claims to be rejected. Staff must review both sides of the patient’s insurance card and confirm eligibility before submitting e-visit claims.
- Incomplete or improper coding: Because e-visits are relatively new, coding errors are common. Using outdated CPT codes, billing for less than the minimum cumulative time requirement, or coding for an e-visit that leads directly to an in-person encounter within seven days are all reasons claims may be denied. Another pitfall is billing for services that require real-time video or in-person evaluation but were coded as asynchronous e-visits.
- Billing and consent errors: E-visits must be initiated by the patient. Billing for unsolicited portal messages, proactive provider check-ins, or reminders not requested by the patient is non-compliant. Practices must also secure clear, documented patient consent to perform the e-visit and inform patients that cost-sharing applies. Failure to capture this consent may trigger audits or repayment requests.
- Administrative and compliance issues: Timely filing is another source of denials. Insurers have strict deadlines for claims submission, and missing them results in lost revenue. In addition, state and federal telehealth regulations change frequently, as do payer-specific policies. Clinicians who do not stay current risk submitting non-compliant claims. Duplicate billing, where the same service is inadvertently submitted twice, is another avoidable but costly mistake.
Preventing pitfalls
The first step in CBT-I billing is identifying the correct CPT codes. Different code series are used; some providers report evaluation and management (E/M) codes for new and established patients. The psychotherapy code set may also be reported; these codes may be reported as a standalone or with an E/M code, if the patient is seen for a medical E/M service on the same day as the psychotherapy session by the same physician or qualified health care professional. The two services must be significant and separately identifiable to report both a psychotherapy session and an E/M. The services are reported by using codes specific to psychotherapy when performed with an E/M service, as an add-on code to the E/M service.
CPT codes for reporting CBT-I
CMS recognizes e-visits as an online digital evaluation and management (E/M) service for established patients. CPT and HCPCS codes distinguish physician/qualified health care professionals from non-physician professional services.
Physicians and qualified health care professionals
These include physicians, nurse practitioners, physician assistants, and clinical nurse specialists. For these clinicians, the following CPT codes apply:
- 99421: Online digital E/M service, 5 to 10 minutes cumulative time over seven days
- 99422: 11 to 20 minutes cumulative time over seven days
- 99423: 21 or more minutes cumulative time over seven day
Qualified non-physician health care professionals
These codes are for professionals such as physical therapists, occupational therapists, speech-language pathologists, licensed clinical psychologists, licensed clinical social workers, and registered dietitians. They use online digital assessment and management service codes:
- 98970: 5 to 10 minutes cumulative time over seven days
- 98971: 11 to 20 minutes cumulative time over seven days
- 98972: 21 or more minutes cumulative time over seven days
Key billing rules
- Established patients only: The patient must be 18 years or older and have an existing relationship with the health care professional.
- Patient-initiated: The e-visit must begin with a patient request through the portal.
- Consent required: Patients must be informed and consented to, with applicable co-pays.
- No overlap with in-person visits: If the e-visit results in an in-person or video encounter for the same condition within seven days, the e-visit should not be billed separately.
- Minimum time threshold: To bill the lowest level code, you must have at least 5 minutes of cumulative time over a seven-day period.
- Place of service: Use the place of service code that would have applied had the service been delivered in person.
- Global period considerations: Do not report e-visits for conditions already covered under a global surgical period.
These codes are designed to reflect the cumulative time spent over seven days, meaning clinicians must carefully document their time, including reviewing the patient’s message, records, and labs, and then crafting a response.
Patient use case
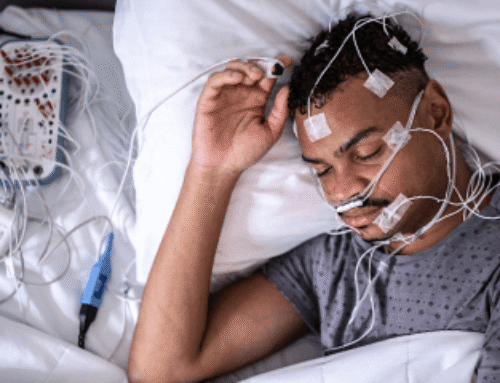
Mr. Johnson, 58, with a history of obstructive sleep apnea managed by CPAP, reports increased fatigue and morning headaches. Instead of an in-person visit, he uses the patient portal to send a secure message, complete a symptom questionnaire, and upload CPAP adherence data. The clinician reviews the information, identifies likely mask leakage, and advises a new mask fitting via portal message. The interaction totals 15 minutes over seven days. CPT 99422 is appropriate for billing.
Conclusion
E-visits offer a flexible, patient-centered approach to care by enabling asynchronous digital communication, which improves access and efficiency, especially during emergencies like the COVID-19 pandemic. However, their success depends on proper billing and compliance, including patient initiation, consent, time thresholds, and accurate coding. To avoid denials and reduce administrative burden, organizations should train staff, streamline workflows, and ensure documentation meets requirements. As e-visits become a permanent fixture in hybrid health care, clinicians who master both clinical and billing aspects will enhance patient access, satisfaction, and practice performance.
This article appeared in volume 11, issue 1 of Montage magazine.