The AASM has sunset its initiative to evaluate coverage policies for diagnostic sleep testing services, and the AASM Payer Policy Review Committee is now shifting its focus to other areas of need, including payer coverage of medications for patients with hypersomnia, payer requirements for accreditation of sleep facilities, and actigraphy reimbursement. The final scores for the 51 diagnostic testing policies reviewed by the committee are displayed on the payer policy scorecards webpage.
The Payer Policy Review Committee developed a payer policy scorecard to evaluate how effective payers are at establishing appropriate coverage policies for diagnostic sleep testing services and to encourage payers to align with the AASM evidence-based recommendation in the “Clinical practice guideline for diagnostic testing for adult obstructive sleep apnea.” The committee described the background and scorecard development process, and summarized the impact of the initiative as of 2020, in the article, “Addressing gaps between payer policies and AASM clinical practice guidelines using scorecards,” published in the Journal of Clinical Sleep Medicine.
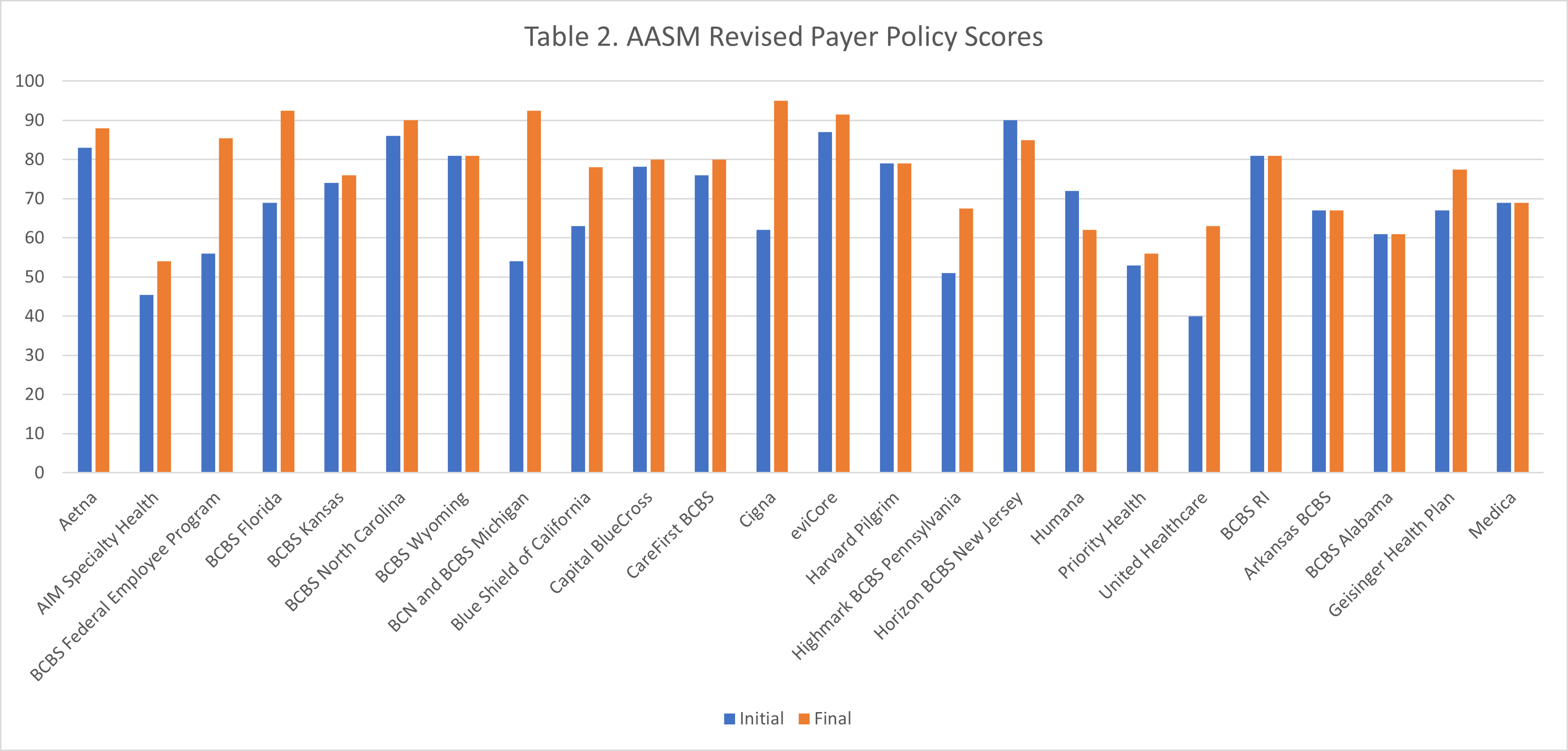
Table 1 shows the total number of policies reviewed and their final scores. Table 2 shows the improvement in scores for all revised policies after re-scoring. The average score for the originally scored policies is 69.2, while the average score for the 22 revised and rescored policies is 78.4, demonstrating the positive impact of this initiative in influencing payers to adopt evidence-based recommendations. The committee thanks the payers who engaged in this effort and the members who reviewed and scored policies, making this initiative a success.
The AASM will continue to respond to other payer issues affecting our members, such as our ongoing advocacy with Blue Shield of California. Send your questions and concerns about payer policies to the AASM health policy team at coding@aasm.org.
Table 1. Total number of diagnostic testing policies reviewed and their final scores
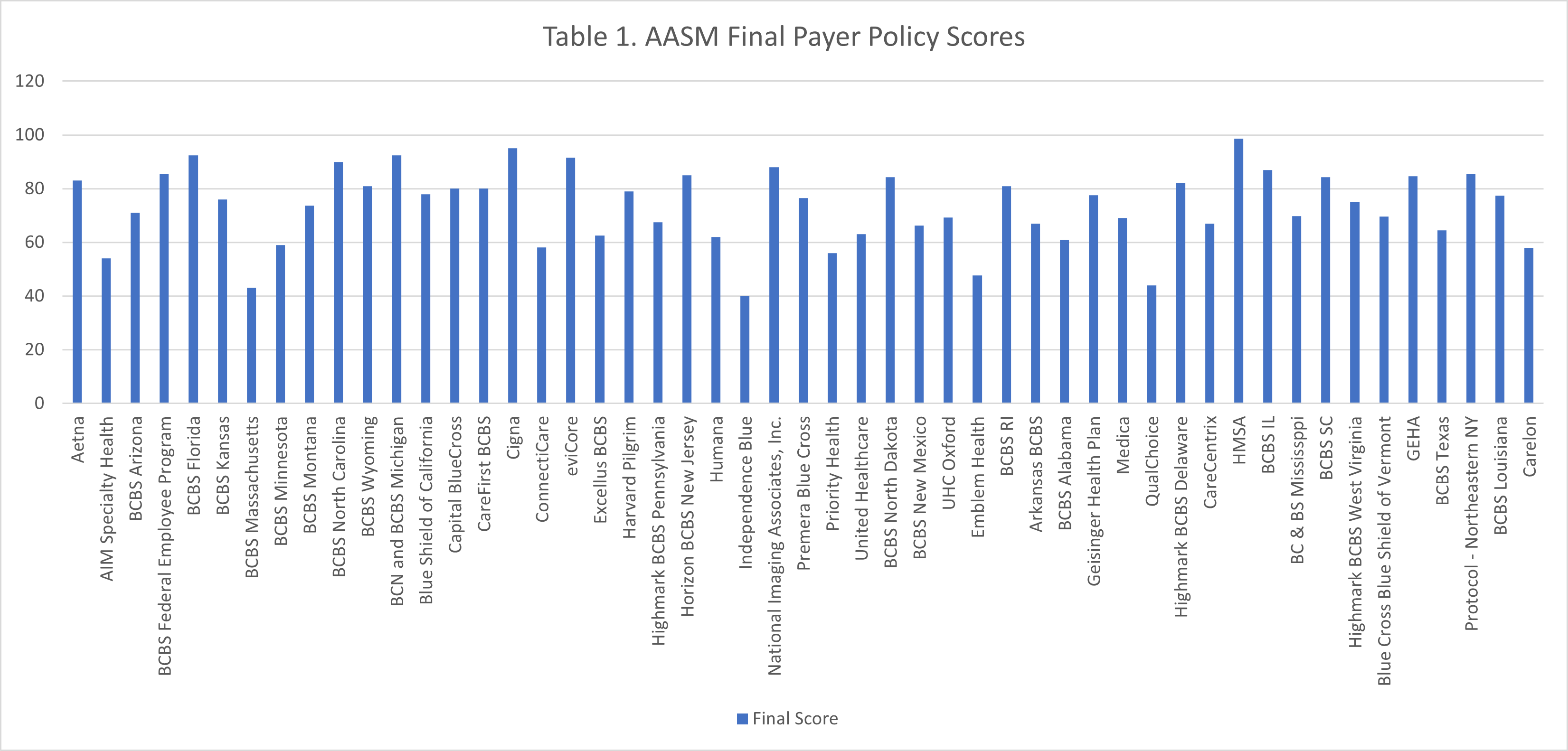
Table 2. Improvement in scores for all revised policies after re-scoring